A Primary Healthcare Nurse’s Guide for Parents and Caregivers
As a primary healthcare nurse, one of the most common—and most serious—concerns I see at the clinic is dehydration in little ones. Between tummy bugs, fevers, and babies’ inability to tell us when they are thirsty, this is something that keeps many parents up at night.
In this guide, I will walk you through exactly how to spot dehydration early, what to do at home, and when to seek medical help.
Why Are Babies and Children at Higher Risk of Dehydration?
Before we look at the signs, it helps to understand why the smallest members of our families are the most vulnerable.
- Higher Water Percentage: A newborn’s body is about 75% water, compared to 55% in adults. This means they have less reserve to draw from when fluid is lost.
- Higher Metabolic Rate: Children use water faster simply because their bodies are growing and working hard.
- Kidney Immaturity: A baby’s kidneys are not as good at conserving water as an adult’s, so they lose more fluid when they urinate.
- Dependence on Others: A toddler cannot pour themselves a glass of water, and a sick baby cannot tell you their mouth is dry. They rely entirely on us to offer fluids.
What Causes Dehydration in Children?
Dehydration happens when fluid leaving the body exceeds fluid intake. The most common causes include:
- Gastroenteritis (Tummy Bug): Vomiting and diarrhoea are the leading causes of dehydration in children.
- Fever: A high fever increases breathing rate and sweating, causing rapid fluid loss.
- Hot Weather: Children lose water quickly through sweat, especially if they play outdoors.
- Sore Throat or Mouth Ulcers: If it hurts to swallow, a child will often refuse to drink.
- Not Drinking Enough: Sometimes, it is simply a busy day, and they forget to take a water break.
Signs of Dehydration in Children: From Mild to Severe
Knowing the signs is your superpower as a parent. Catching it early makes all the difference.
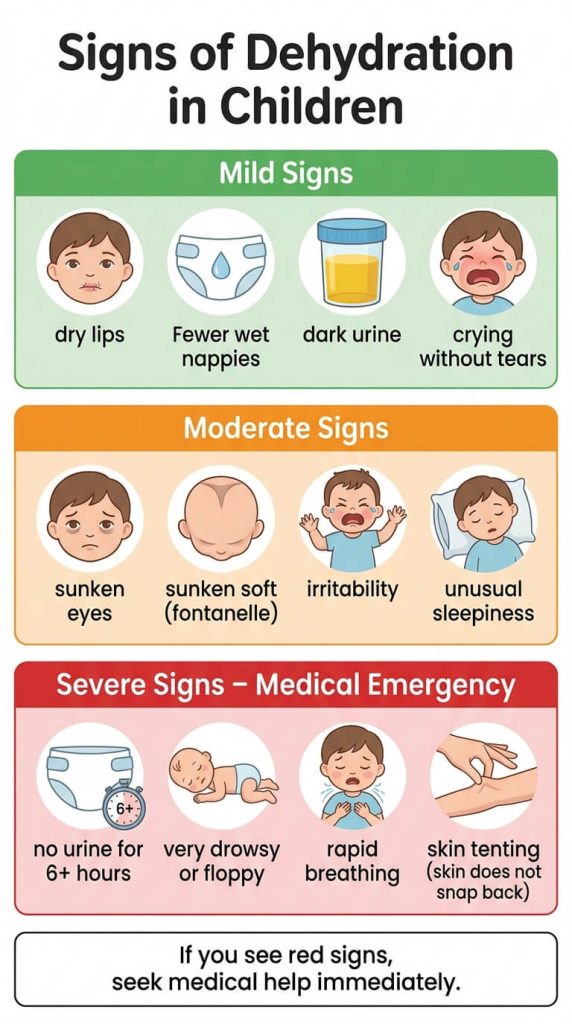
Early Signs (Mild to Moderate)
- Dry, cracked lips and a sticky or dry mouth
- Fewer wet nappies than usual (fewer than 4 wet nappies in 24 hours for an infant)
- Dark, strong-smelling urine (healthy urine should be pale yellow)
- Crying without tears
- Sunken eyes
- Sunken soft spot (fontanelle) on top of the baby’s head
- Irritability, fussiness, or unusual sleepiness
Severe Dehydration – This Is a Medical Emergency
If you see any of the following signs, do not try to treat them at home. Go to your nearest clinic or emergency room immediately:
- No urine for 6–8 hours for an infant, or 12 hours for a toddler
- Very drowsy, floppy, or hard to wake up
- Rapid breathing or a fast heartbeat
- Purple or blue lips
- Skin pinch test: When you gently pinch the skin on their tummy, it does not snap back quickly; it stays “tented”.
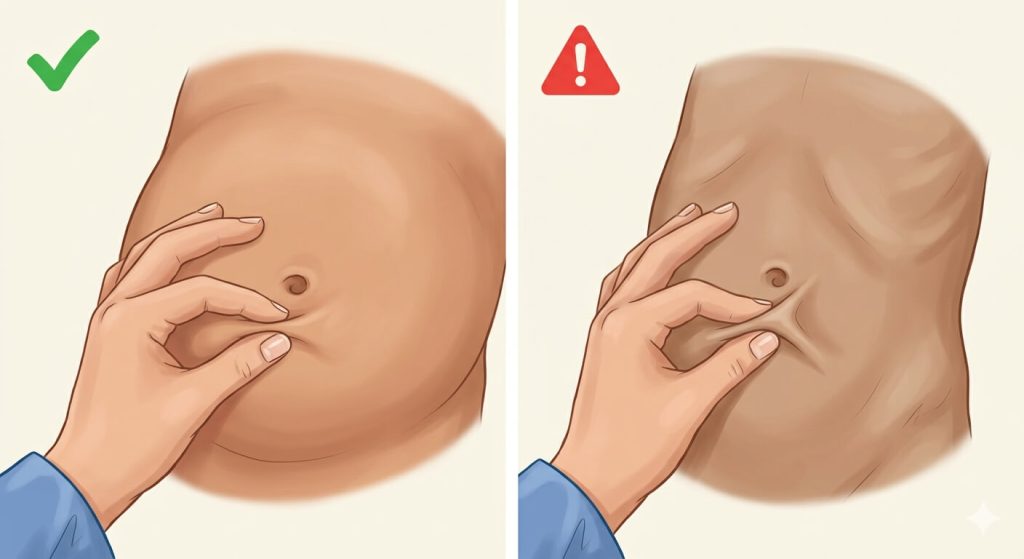
A Nurse’s Guide: How to Rehydrate Your Child
How you rehydrate depends on your child’s age and the cause of the dehydration.
Important: What NOT to Give
- Babies under 6 months: Do not give plain water. It can dilute their sodium levels and cause a dangerous imbalance.
- Avoid sugary drinks: Soft drinks, fruit juices, and sports drinks are not ideal for rehydration. They often have too much sugar and not enough salt. The high sugar content can actually worsen diarrhoea by drawing more water into the bowel.
- The Salt and Sugar Remedy: While homemade sugar-salt solutions are sometimes used, they must be mixed with extreme accuracy. Commercial oral rehydration solutions (ORS) are safer, more reliable, and readily available at pharmacies and clinics.
Rehydration by Age Group
Babies Under 6 Months
Your first line of defence is breastmilk or formula. Breastmilk is naturally hydrating and contains the perfect balance of electrolytes.
- If breastfeeding, feed more frequently. Offer the breast every 15–20 minutes if possible.
- If formula feeding, offer smaller amounts of formula more often.
- When to use ORS: If the baby is showing mild signs of dehydration and is vomiting or has diarrhoea, you can use an oral rehydration solution (ORS) available from your local pharmacy or clinic.
- Nurse’s Tip: Offer the ORS by teaspoon every 5–10 minutes rather than a full bottle, which might trigger vomiting.
Babies Over 6 Months and Toddlers
- Oral Rehydration Solution (ORS): This is the gold standard. Buy ORS sachets from your local pharmacy or clinic. Mix exactly according to the packet instructions.
- Homemade Solution (If You Have No ORS): Mix 1 litre of clean, safe water with 6 level teaspoons of sugar and ½ level teaspoon of salt. Stir well.
- Offer small, frequent sips: A straw, a syringe (without the needle), or a spoon can help if they are refusing a cup.
- Continue milk feeds: You can continue breastfeeding or formula alongside the ORS.
A Practical Guide to Oral Rehydration
Oral rehydration therapy works because of a specific balance of sugar and salt that helps the gut absorb water. Here is how to do it right:
| Age Group | Fluid of Choice | How to Give It |
| Under 6 months | Breast milk or Formula (more frequently) | If vomiting, give small amounts every 10 minutes via spoon |
| 6 months – 2 years | Oral Rehydration Solution (ORS) | Offer 1–2 teaspoons every 5–10 minutes |
| Over 2 years | Oral Rehydration Solution, Clear Broth, or Water | Small sips every 5 minutes. If they keep it down, increase slowly |
The “Sip” Rule
The “Sip” Rule
The golden rule for rehydrating a vomiting child is “small, frequent sips”. Do not let them chug a large cup of fluid. They will likely vomit it right back up.
- Start with 1 teaspoon every 5 minutes
- If they keep that down for an hour, increase to 1 tablespoon every 5 minutes
When to See a Doctor
You have started rehydrating, but when is it time to stop and get help?
- Your baby is under 6 months and has any signs of dehydration
- Your child cannot keep any fluids down for more than 4 hours
- Vomiting or diarrhoea persists for more than 24 hours
- Signs of dehydration worsen (they become more lethargic, have fewer wet nappies, or become more irritable)
- There is blood in the vomit or stool
- Your child has a weakened immune system or another underlying condition
Preventing Dehydration
Prevention is always better than a cure. Here is how to keep little bodies hydrated:
- Serve water at meals: Make it a habit from an early age
- Carry a water bottle: Whether it is a trip to the shop or the park, always have water on hand
- Be proactive during illness: If your child has a fever or is vomiting, do not wait for them to ask for water. Offer small amounts regularly
- Avoid sugary drinks: They can actually make dehydration worse in the long run
- Dress appropriately: In hot weather, dress your child in light, breathable clothing to prevent excessive sweating
Frequently Asked Questions by Parents
Q: How can I tell if my baby is dehydrated just by looking at their nappy?
A: A well-hydrated baby should have a wet nappy every 4–6 hours. If you notice fewer than 4 wet nappies in 24 hours or the urine is dark and has a strong smell, treat it as a warning sign.
Q: Can I give my baby water if it is very hot outside?
A: If your baby is under 6 months and exclusively breastfed, breast milk is sufficient hydration, even in hot weather. Formula-fed babies can have small amounts of cooled, boiled water (about 30–60ml) between feeds, but do not replace feeds with water. Once solids are introduced (around 6 months), water can be offered regularly.
Q: Is oral rehydration solution (ORS) safe for my toddler?
A: Yes, ORS is safe and effective for toddlers. Just ensure you follow the mixing instructions exactly. Too much water dilutes it, and too little water can be harmful.
Q: Should I stop feeding my child if they have diarrhoea?
A: No. This is an old myth. You should continue to feed your child. Breastfeeding should continue, and older children should return to their normal diet as soon as they are rehydrated. Food helps the gut heal.
Final Words from a Nurse
Dehydration can be frightening, but with the right knowledge, you can manage mild cases at home and know exactly when to seek help. Trust your instincts. If something feels wrong, it is always better to have your child checked by a healthcare professional.
You are doing a wonderful job caring for your little one.
Nurse K is a practising PHC nurse in South Africa. She writes anonymously to help busy mums raise healthy little ones. Real advice. No jargon. No judgement.
Medical Disclaimer
Medical Disclaimer
The information provided on BusyMumsWorld is for general informational and educational purposes only. This website does not constitute medical advice, diagnosis, or treatment.
About Me
I am a registered nurse with the South African Nursing Council (SANC). I draw upon my nursing training and clinical experience to provide helpful, evidence-informed information for mothers, babies, and families. However, my role on this website is that of an educator and content creator, not your personal healthcare provider.
No Nurse-Patient Relationship
Your use of this website does not create a nurse-patient relationship between you and me. The content on this site does not replace an in-person clinical assessment, physical examination, or professional medical consultation. In accordance with the Nursing Act, 2005 (Act No. 33 of 2005) and the SANC Code of Ethics, I clearly distinguish between my role as a registered nurse in clinical practice and my role as a content creator.
For Babies and Children
Content related to infant and child health is for educational purposes only. Every child is unique. What works for one child may not be appropriate for another. Always consult your paediatrician, clinic sister, family doctor, or other qualified healthcare provider regarding any medical concerns about your child, including changes in behaviour, feeding, sleep, growth, or physical symptoms.
For Mothers
Content related to pregnancy, antenatal care, postpartum recovery, breastfeeding, and maternal health is for educational purposes only. Your healthcare needs are individual and may change during pregnancy and the postnatal period. Always seek guidance from your doctor, midwife, obstetrician, lactation consultant, or local clinic for any questions about your or your baby’s health.
South African Context
Where possible, I aim to provide information relevant to the South African healthcare context, including public and private healthcare considerations. However, healthcare resources, protocols, and availability may vary by province, facility, and individual circumstance. Always confirm information with your own healthcare provider.
SANC Compliance
In compliance with the rules and ethical guidelines of the South African Nursing Council (SANC):
- I clearly state that the information on this site does not constitute the practice of nursing as defined in the Nursing Act
- I do not offer individualised nursing assessments, diagnoses, or treatment plans through this website
- I encourage all readers to seek in-person care from registered healthcare professionals for their specific health needs
- I maintain professional boundaries by not providing specific medical advice in response to comments, emails, or messages
Emergency Warning
If you or your child is experiencing a medical emergency, do not use this website for advice. Call emergency services immediately. Alternatively, go to your nearest hospital emergency department, clinic, or doctor immediately.
Do not delay seeking emergency care because of something you have read on this website.
Limitation of Liability
I make every effort to ensure the accuracy of the information published on this site. However, medical knowledge is constantly evolving, and information may become outdated. I cannot guarantee that all information is complete, current, or accurate for every individual circumstance. I assume no responsibility or liability for any errors or omissions in the content of this site. Your use of this website is at your own risk.
Affiliate Disclosure
BusyMumsWorld participates in affiliate marketing programmes. This means that some links on this site may be affiliate links. If you choose to purchase through these links, I may earn a small commission at no additional cost to you.
My Commitment to You
I am a registered nurse with the South African Nursing Council (SANC). My recommendations are based on my professional knowledge, clinical experience, and genuine belief that a product may be helpful to my audience. Affiliate partnerships do not influence my clinical judgement, the information I provide, or my commitment to evidence-based content.
Important Note
Products mentioned on this site are for informational purposes only. If a product makes medical claims, please consult your doctor, paediatrician, or other qualified healthcare provider before use. My nursing credentials do not constitute an endorsement of any specific product, and I do not receive compensation for clinical recommendations.
Last Updated: March 2026

