Your toddler wakes up at 11 pm crying, pulling at their ear, and refusing to settle. Your mind races: Is it an ear infection? Teething? Something stuck in there? Do we need to go to the emergency room tonight?
As a primary healthcare nurse, I have seen this exact situation countless times. Ear pain in children is one of the most common reasons parents lose sleep.
This guide will help you answer one question tonight:
Do I wait, go in the morning, or go now?
When Should You Worry About Ear Pain in a Child? (Quick Answer)
You should seek urgent medical care if your child:
- Is under 6 months with ear pain
- Has a fever above 38.5°C that is not settling
- Has swelling or redness behind the ear
- Has discharge (pus or fluid) from the ear
- Is very sleepy or hard to wake
- Has a stiff neck or seizure
Quick Ear Pain Checklist (Save This)
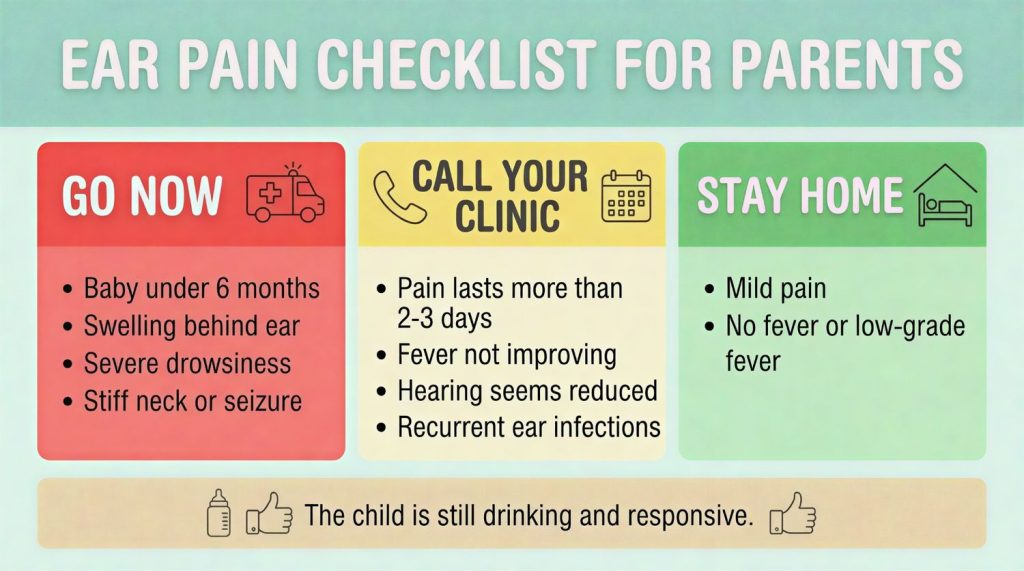
🔴 GO NOW:
- Swelling behind the ear
- Severe drowsiness
- Stiff neck or seizure
- Baby under 6 months
🟡 Go in the morning:
- Pain lasts more than 2–3 days
- Fever not improving
- Hearing seems reduced
- Recurrent ear infections
🟢 STAY HOME:
- Mild pain
- No fever or low-grade fever
- The child is still drinking and responsive
Ear Pain vs Teething – How to Tell the Difference
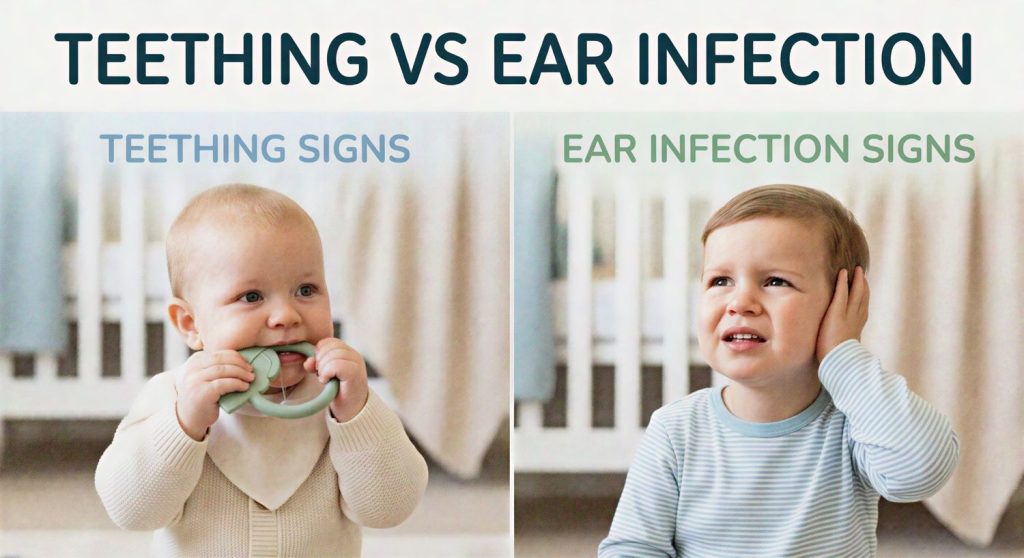
Teething:
- Drooling
- Chewing on objects
- Mild fussiness
- Fever below 38.5°C
Ear Infection:
- Fever above 38.5°C
- Pulling at the ear
- Poor sleep (worse lying down)
- Cold symptoms (runny nose, cough)
Key rule:
If there is a high fever + cold symptoms + ear pulling → think ear infection, not teething.
The 3 Main Causes of Ear Pain in Children
1. Middle Ear Infection (Most Common)
Usually follows a cold. Fluid builds up behind the eardrum.
Signs:
- Fever
- Night waking
- Ear pulling
- Irritability
2. Glue Ear (Fluid Without Infection)
No pain, but it affects hearing.
Signs:
- Not responding to sounds
- Turning the volume up
- Speech delay (if long-term)
3. Swimmer’s Ear (Outer Ear Infection)
Infection in the ear canal.
Signs:
- Pain when touching the ear
- Itching
- Redness
Simple Home Checks You Can Do
- An ear tug hurts, likely an outer ear infection
- No pain on touch, likely a middle-ear infection
How to Manage Ear Pain at Home
When your child has ear pain, it can be distressing for both of you—especially at night when the pain often feels worse. The good news is that many ear infections can be managed comfortably at home while the body heals.
Start with pain relief, because controlling pain is the most important step. Medications like paracetamol or ibuprofen can help reduce both pain and fever. These should be given according to your clinic’s advice or the correct dose for your child’s age and weight. Once the pain is under control, children usually settle, eat better, and rest more easily.
Positioning also makes a difference. Try to keep your child upright or slightly elevated, especially during feeds or sleep. Lying completely flat can increase pressure in the middle ear, which may worsen the discomfort. Even holding your child against your chest in an upright position can bring noticeable relief.
A simple warm compress can be surprisingly soothing. Placing a warm (not hot) cloth over the affected ear may help ease the pain and provide comfort. It’s not a cure, but it can calm a distressed child, especially when combined with pain medication.
Don’t underestimate the value of fluids and rest. Encourage your child to drink regularly—whether it’s water, breastmilk, or formula—because swallowing can help the ear naturally drain and equalise pressure. Rest is just as important; the body needs energy to fight off the infection, so allow your child to sleep as much as they need.
Finally, it’s important to avoid putting anything into the ear. This includes cotton buds, oils, or home remedies. The ear is delicate, and inserting anything can cause irritation or even injury, especially if the eardrum is inflamed.
With these simple measures, most children start to feel better within a couple of days—even without antibiotics.
When to Visit the Clinic
Go to your GP or clinic if:
- Pain lasts more than 2–3 days
- The fever continues
- Discharge from the ear
- Hearing seems reduced
- Child under 6 months
Red Flags – When to Go to the Emergency Room
- Swelling behind the ear
- Stiff neck
- Very sleepy child
- Seizure
- Breathing difficulty
Why Ear Pain Is Worse at Night
Ear pressure increases when lying down.
This makes the inflamed eardrum more painful.
It feels worse—but it does NOT always mean it’s getting worse.
Can Ear Infections Go Away on Their Own?
Yes. Most ear infections start to improve within 2–3 days without antibiotics, although full recovery may take a little longer.
Prevention Tips
- Breastfeed if possible
- Avoid smoke exposure
- Keep vaccines up-to-date.
- Reduce dummy use after 6 months
Frequently Asked Questions
Does my child need antibiotics?
Not always. Many infections are viral and clear on their own.
Can teething cause ear pain?
Yes, but not a high fever.
Can my child swim?
Yes, for middle ear infections; no, if discharge is present.
Should I use cotton buds?
Never.
If you enjoyed this article, you might like:
Baby Won’t Stop Crying: Causes, Soothing Tips & When to Worry
Fever in Children: The “Wait or Worry” Checklist
Baby Symptoms Guide: What’s Normal & When to Worry (A Nurse’s Guide for Parents)
Nurse K is a practising PHC nurse in South Africa. She writes anonymously to help busy mums raise healthy little ones. Real advice. No jargon. No judgement.
Medical Disclaimer
Medical Disclaimer
The information provided on BusyMumsWorld is for general informational and educational purposes only. This website does not constitute medical advice, diagnosis, or treatment.
About Me
I am a registered nurse with the South African Nursing Council (SANC). I draw upon my nursing training and clinical experience to provide helpful, evidence-informed information for mothers, babies, and families. However, my role on this website is that of an educator and content creator, not your personal healthcare provider.
No Nurse-Patient Relationship
Your use of this website does not create a nurse-patient relationship between you and me. The content on this site does not replace an in-person clinical assessment, physical examination, or professional medical consultation. In accordance with the Nursing Act, 2005 (Act No. 33 of 2005) and the SANC Code of Ethics, I clearly distinguish between my role as a registered nurse in clinical practice and my role as a content creator.
For Babies and Children
Content related to infant and child health is for educational purposes only. Every child is unique. What works for one child may not be appropriate for another. Always consult your paediatrician, clinic sister, family doctor, or other qualified healthcare provider regarding any medical concerns about your child, including changes in behaviour, feeding, sleep, growth, or physical symptoms.
For Mothers
Content related to pregnancy, antenatal care, postpartum recovery, breastfeeding, and maternal health is for educational purposes only. Your healthcare needs are individual and may change during pregnancy and the postnatal period. Always seek guidance from your doctor, midwife, obstetrician, lactation consultant, or local clinic for any questions about your or your baby’s health.
South African Context
Where possible, I aim to provide information relevant to the South African healthcare context, including public and private healthcare considerations. However, healthcare resources, protocols, and availability may vary by province, facility, and individual circumstance. Always confirm information with your own healthcare provider.
SANC Compliance
In compliance with the rules and ethical guidelines of the South African Nursing Council (SANC):
- I clearly state that the information on this site does not constitute the practice of nursing as defined in the Nursing Act
- I do not offer individualised nursing assessments, diagnoses, or treatment plans through this website
- I encourage all readers to seek in-person care from registered healthcare professionals for their specific health needs
- I maintain professional boundaries by not providing specific medical advice in response to comments, emails, or messages
Emergency Warning
If you or your child is experiencing a medical emergency, do not use this website for advice. Call emergency services immediately. Alternatively, go to your nearest hospital emergency department, clinic, or doctor immediately.
Do not delay seeking emergency care because of something you have read on this website.
Limitation of Liability
I make every effort to ensure the accuracy of the information published on this site. However, medical knowledge is constantly evolving, and information may become outdated. I cannot guarantee that all information is complete, current, or accurate for every individual circumstance. I assume no responsibility or liability for any errors or omissions in the content of this site. Your use of this website is at your own risk.
Affiliate Disclosure
BusyMumsWorld participates in affiliate marketing programmes. This means that some links on this site may be affiliate links. If you choose to purchase through these links, I may earn a small commission at no additional cost to you.
My Commitment to You
I am a registered nurse with the South African Nursing Council (SANC). My recommendations are based on my professional knowledge, clinical experience, and genuine belief that a product may be helpful to my audience. Affiliate partnerships do not influence my clinical judgement, the information I provide, or my commitment to evidence-based content.
Important Note
Products mentioned on this site are for informational purposes only. If a product makes medical claims, please consult your doctor, paediatrician, or other qualified healthcare provider before use. My nursing credentials do not constitute an endorsement of any specific product, and I do not receive compensation for clinical recommendations.
Last Updated: March 2026
