You walk into your baby’s room for their morning feed, and your heart stops. Your little one has red eyes – one or both eyes look pink, swollen, and crusted with yellow discharge. Red eyes in babies can be frightening, but most cases are not serious. Your mind races: Is this an infection? Is it contagious? Do I need to go to the emergency room?
Red eyes in babies are extremely common and usually not serious. As a primary healthcare nurse, I have seen hundreds of parents panic over a red, gunky eye. The good news is that most cases are either a mild infection (conjunctivitis), a blocked tear duct, or simple irritation.
In this guide, I will help you tell hioiythe diffelkjrence between conjunctivitis and irritation, show you how to clean your baby’s eyes safely, and give you the red flags that mean it is time to see a doctor.
What Parents Ask Most About Red Eyes in Babies
Parents have many questions when they notice red eyes in their baby. Here are the most common concerns answered simply and clearly.
How can I tell if my baby has conjunctivitis or just irritation?
The key is looking at the discharge and whether one or both eyes are affected. Conjunctivitis usually causes thick, yellow-green discharge that keeps coming back. Irritation causes watery eyes that clear up once the irritant is removed.
Is it safe to treat red eyes in babies at home?
For mild cases of irritation or a blocked tear duct, home care is fine. But if you see thick discharge or swelling or your baby seems unwell, see a doctor.
How long does baby conjunctivitis last?
Viral conjunctivitis lasts 5–7 days. Bacterial conjunctivitis improves within 24–48 hours of starting antibiotic drops.
Is my baby’s red eye contagious?
Bacterial and viral conjunctivitis are highly contagious. Irritation and blocked tear ducts are not contagious.
Can teething cause red eyes in babies?
No. Teething does not cause red eyes. This is a common myth. If your teething baby has red eyes, they have another cause.
Conjunctivitis vs Irritation: Quick Comparison Table
This table helps you tell the difference at a glance:
| Feature | Conjunctivitis (Infection) | Irritation / Blocked Tear Duct |
|---|---|---|
| Discharge colour | Yellow, green, or thick white | Clear and watery |
| Discharge texture | Sticky, crusty, dries on lashes | Thin, runs down cheek |
| One or both eyes? | Often starts in one, spreads to both | Usually one eye (blocked duct) or both (irritation) |
| Swelling | Yes – eyelids may be puffy | Minimal or none |
| Redness | Bright red or pink | Mild pink |
| Does baby seem unwell? | May have fever, be fussy, and feed poorly | Happy, feeding normally |
| Contagious? | Yes (bacterial and viral) | No |
| Common age | Any age | Blocked ducts: birth to 12 months |
Bacterial vs Viral Conjunctivitis in Babies
Not all conjunctivitis is the same. Here is how to tell the difference:
Bacterial Conjunctivitis
| Sign | What to Look For |
|---|---|
| Discharge | Thick, yellow-green, sticky |
| Eye appearance | Eyelashes may be stuck together, especially after sleep |
| Onset | Sudden |
| Affected eyes | Often starts in one eye, spreads to the other |
| Treatment | Antibiotic eye drops from a doctor |
Viral Conjunctivitis
| Sign | What to Look For |
|---|---|
| Discharge | Watery, clear or white |
| Eye appearance | Red and watery, less sticky than bacterial |
| Onset | Gradual, often with cold symptoms |
| Affected eyes | Often both eyes at the same time |
| Treatment | Supportive care – antibiotics do not work on viruses |
Blocked Tear Ducts in Newborns: A Common Cause of Red Eyes in Babies
This is one of the most common causes of red eyes in babies under 12 months, yet many parents have never heard of it.
What is a blocked tear duct?
Tears normally drain through a small tube (tear duct) from the eye to the nose. In about 1 in 5 newborns, this tube is narrow or blocked. The tears have nowhere to go, so they build up and spill out.
Signs of a blocked tear duct:
- Constant watery eye (looks like the baby is always crying)
- Mild redness around the inner corner of the eye
- Clear or white discharge (not yellow or green)
- Symptoms are worse in the morning or when the baby has a cold
- No fever – baby acts completely normal
Does it need treatment?
Most blocked tear ducts resolve on their own by 12 months of age. You do not need antibiotics unless the eye becomes truly infected (yellow-green discharge, swelling).
Home care for a blocked tear duct:
Gently massage the inner corner of the eye (near the nose) 2–3 times per day. Your doctor or health visitor can show you how.
When It’s Just Irritation (Not Conjunctivitis)
Sometimes red eyes in babies have nothing to do with infection. Common irritants include:
| Irritant | What to Do |
|---|---|
| Dry air | Use a cool-mist humidifier in the baby’s room |
| Smoke | Keep the baby away from cigarette smoke, fireplaces, and candles |
| Chlorine | Rinse eyes with clean water after swimming |
| Soap or shampoo | Rinse thoroughly; avoid getting soap in eyes |
| Dust or pet dander | Vacuum regularly, wash bedding |
| Foreign object (dust, sand, eyelash) | Rinse with clean water or saline drops |
| Rubbing eyes | Keep baby’s nails short; distract with toys |
Irritation usually resolves within a few hours of removing the cause. If red eyes persist beyond 24 hours, consider another cause.
Home Care: How to Clean Your Baby’s Eyes Safely
Whether your baby has conjunctivitis or irritation, proper cleaning helps. Here is the safe technique.
Wash your hands thoroughly with soap
Dip a cotton ball into cooled, boiled water
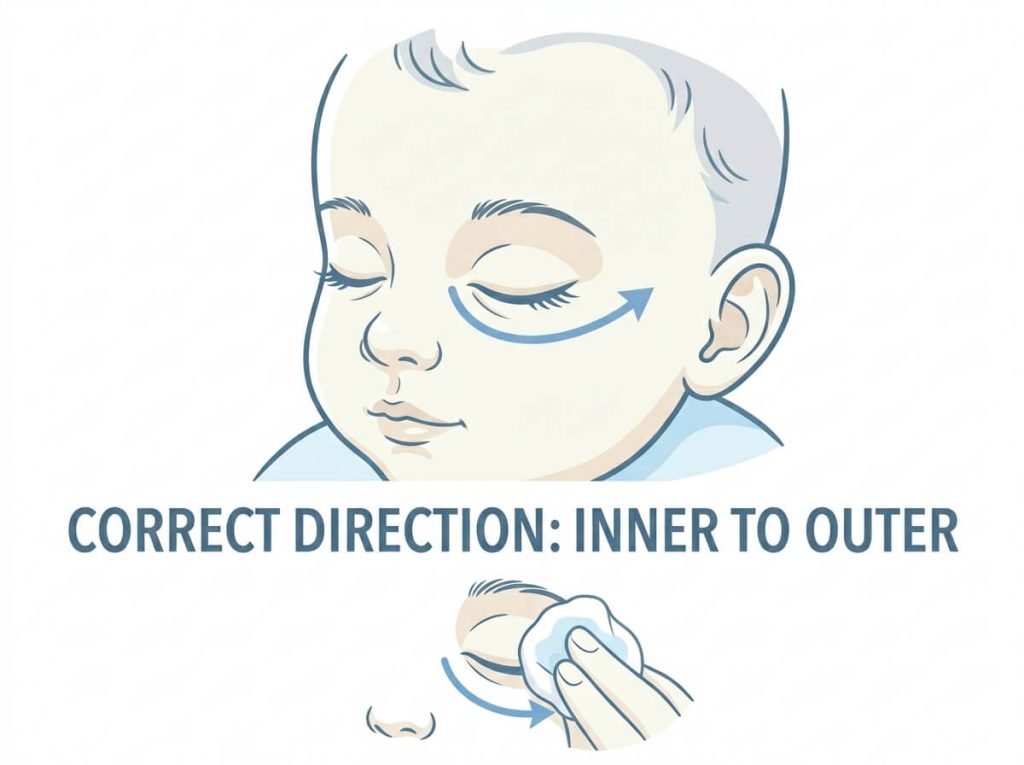
Wipe from the inner corner of the eye (near the nose) outwards
Use a fresh cotton ball for each wipe
Repeat until the eye looks clean
Use a new cotton ball for the other eye
Wash your hands again afterwards
Important safety rules:
| Do | Don’t |
|---|---|
| Use a fresh cotton ball for each wipe | Reuse cotton balls |
| Wash your hands before and after | Wipe back and forth (can spread infection) |
| Touch your own eyes while caring for the baby | Touch your own eyes while caring for baby |
| Use cooled, boiled water | Use tap water directly |
Red Flags: When to See a Doctor for Red Eyes in Babies
Most red eyes in babies can be managed at home. But sometimes you need medical help.
See a doctor within 24 hours if:
| Red Flag | Why |
|---|---|
| Thick yellow or green discharge | Likely bacterial conjunctivitis needing antibiotics |
| Eye swelling that is getting worse | May be spreading infection |
| The baby seems unwell, fussy, or has a fever | Could be a more serious illness |
| Redness spreads to the skin around the eye (like a black eye) | Could be periorbital cellulitis – a medical emergency |
| Symptoms not improving after 48 hours of home care | Needs proper diagnosis |
Seek emergency care immediately if:
| Red Flag | What It Could Mean |
|---|---|
| The baby cannot open their eye | Severe swelling or infection |
| Bulging eye | Orbital cellulitis – seek emergency care |
| Changes in vision (baby not following faces or toys) | Serious eye problem |
| The baby is very unwell, lethargic, or not feeding | Systemic illness |
| Green discharge with fever in a newborn under 4 weeks | Newborn conjunctivitis requires urgent treatment |
Can My Baby Go to Nursery with Red Eyes?
This depends on the cause:
| Cause | Can They Attend? | When Can They Return? |
|---|---|---|
| Blocked tear duct | Yes | Not contagious – no restrictions |
| Irritation | Yes | Not contagious – no restrictions |
| Viral conjunctivitis | No | When eyes are no longer red and watery (usually 5–7 days) |
| Bacterial conjunctivitis | No | After 24 hours of antibiotic treatment AND discharge has stopped |
Always check your nursery’s policy. Many require a doctor’s note before returning after conjunctivitis.
Myth Busting: What Does NOT Cause Red Eyes in Babies
| Myth | Truth |
|---|---|
| Teething causes red eyes | False. Teething does not cause red eyes. If your baby has red eyes, look for another cause. |
| Breast milk cures conjunctivitis | False. Breast milk is not a proven treatment for eye infections. It can introduce bacteria. Use cooled, boiled water or prescribed drops only. |
| Red eyes mean antibiotics every time | False. Viral conjunctivitis and blocked ducts do not need antibiotics. |
| You can share eye drops between siblings | False. Never share eye drops – this spreads infection. |
Related Childhood Illnesses
While you are here, you may find these guides helpful:
- Fever: When red eyes occur with fever
- Dehydration: If your baby is unwell and feeding poorly
- Rising Temperature at Night: Fevers that spike after dark
Final Thoughts on Red Eyes in Babies
Seeing red eyes in babies is frightening, especially when you wake up to a crusted, swollen eye. But here is what I want you to remember: most red eyes in babies are not emergencies.
Red eyes in babies caused by a blocked tear duct will resolve on their own. Red eyes in babies from irritation clear up once the irritant is removed. Even conjunctivitis in babies usually responds well to treatment.
Your job is not to panic. Your job is to look at the discharge, check if the baby seems unwell, clean the eyes safely, and know the red flags that mean it is time to see a doctor.
Keep this guide handy. Trust your instincts. And remember – you have got this.
Nurse K is a practising PHC nurse in South Africa. She writes anonymously to help busy mums raise healthy little ones. Real advice. No jargon. No judgement.
Medical Disclaimer
Medical Disclaimer
The information provided on BusyMumsWorld is for general informational and educational purposes only. This website does not constitute medical advice, diagnosis, or treatment.
About Me
I am a registered nurse with the South African Nursing Council (SANC). I draw upon my nursing training and clinical experience to provide helpful, evidence-informed information for mothers, babies, and families. However, my role on this website is that of an educator and content creator, not your personal healthcare provider.
No Nurse-Patient Relationship
Your use of this website does not create a nurse-patient relationship between you and me. The content on this site does not replace an in-person clinical assessment, physical examination, or professional medical consultation. In accordance with the Nursing Act, 2005 (Act No. 33 of 2005) and the SANC Code of Ethics, I clearly distinguish between my role as a registered nurse in clinical practice and my role as a content creator.
For Babies and Children
Content related to infant and child health is for educational purposes only. Every child is unique. What works for one child may not be appropriate for another. Always consult your paediatrician, clinic sister, family doctor, or other qualified healthcare provider regarding any medical concerns about your child, including changes in behaviour, feeding, sleep, growth, or physical symptoms.
For Mothers
Content related to pregnancy, antenatal care, postpartum recovery, breastfeeding, and maternal health is for educational purposes only. Your healthcare needs are individual and may change during pregnancy and the postnatal period. Always seek guidance from your doctor, midwife, obstetrician, lactation consultant, or local clinic for any questions about your or your baby’s health.
South African Context
Where possible, I aim to provide information relevant to the South African healthcare context, including public and private healthcare considerations. However, healthcare resources, protocols, and availability may vary by province, facility, and individual circumstance. Always confirm information with your own healthcare provider.
SANC Compliance
In compliance with the rules and ethical guidelines of the South African Nursing Council (SANC):
- I clearly state that the information on this site does not constitute the practice of nursing as defined in the Nursing Act
- I do not offer individualised nursing assessments, diagnoses, or treatment plans through this website
- I encourage all readers to seek in-person care from registered healthcare professionals for their specific health needs
- I maintain professional boundaries by not providing specific medical advice in response to comments, emails, or messages
Emergency Warning
If you or your child is experiencing a medical emergency, do not use this website for advice. Call emergency services immediately. Alternatively, go to your nearest hospital emergency department, clinic, or doctor immediately.
Do not delay seeking emergency care because of something you have read on this website.
Limitation of Liability
I make every effort to ensure the accuracy of the information published on this site. However, medical knowledge is constantly evolving, and information may become outdated. I cannot guarantee that all information is complete, current, or accurate for every individual circumstance. I assume no responsibility or liability for any errors or omissions in the content of this site. Your use of this website is at your own risk.
Affiliate Disclosure
BusyMumsWorld participates in affiliate marketing programmes. This means that some links on this site may be affiliate links. If you choose to purchase through these links, I may earn a small commission at no additional cost to you.
My Commitment to You
I am a registered nurse with the South African Nursing Council (SANC). My recommendations are based on my professional knowledge, clinical experience, and genuine belief that a product may be helpful to my audience. Affiliate partnerships do not influence my clinical judgement, the information I provide, or my commitment to evidence-based content.
Important Note
Products mentioned on this site are for informational purposes only. If a product makes medical claims, please consult your doctor, paediatrician, or other qualified healthcare provider before use. My nursing credentials do not constitute an endorsement of any specific product, and I do not receive compensation for clinical recommendations.
Last Updated: March 2026

